Patients and doctors are allies separated by a common language: suffering.
Patients suffer because of their diseases, because of their feelings of alienation within a technocratic medical system and because their experience is ignored in our society that often believes the best way to get rid of suffering is to get rid of the sufferer.
In the face of these obstacles, patients seek physicians not only as experts in treating their illnesses and wounds but also as experts in alleviating their suffering. But are these expectations well founded?
Patients and doctors are allies separated by a common language: suffering.
When I speak at medical conferences, I always ask the physicians, nurses and students if they learned anything about suffering—their own or that of their patients—during their training. Inevitably, no hands go up. Indeed, a 2017 study in Family Medicine found that such education is not taking place even though students want it. An accompanying editorial stated: “To be worthy to serve [suffering patients] means that we first must undertake the study of suffering. We cannot hope to address the phenomenon without exploring it within ourselves, our patients, our communities, our society.”
There is, however, a grievous obstacle, invisible to most patients, that prevents doctors from undertaking “the study of suffering”: Physicians themselves are suffering under the very same health care system as their patients.
Over half of physicians satisfy criteria for burnout: emotional/physical exhaustion, cynicism/depersonalization and/or a lack of sense of accomplishment in patient care.
Electronic health records and increasing government regulations contribute to physician burnout. Due to E.H.R.s, the average physician spends two to three minutes on a computer for each minute spent face-to-face with a patient. Increased government-mandated administrative tasks, though well intentioned, can suck the joy out of physicians who start seeing their profession as a burden, instead of a meaningful calling. Unless this soul-crushing epidemic of physician burnout ends, doctors will not have the emotional energy or motivation to learn about and address their patients’ suffering.
Physicians themselves are suffering under the very same health care system as their patients.
While physician burnout and its solutions are multifaceted issues, the Catholic Medical Association is one innovator that is already addressing suffering among Catholic physicians and their patients.
In 2012, a colleague urged me to write a discussion-based course for health care professionals based on St. John Paul’s apostolic letter, “Salvifici Doloris.” This free course, successfully used since 2014 by an increasing number of our 104 local physician guilds and 34 medical student guilds, teaches physicians how to understand and address their own suffering so they can empathically see their patients as fellow sufferers and learn how to practice compassion.
National and regional conferences, annual diocesan White Masses and local guilds provide places where physicians and students learn how to live the C.M.A. mission “to uphold the principles of the Catholic faith in the science and practice of medicine.” Most important, in an age when the very definition of “person” seems up for grabs, a guild is a place where we learn how to become a certain kind of person: a physician inspired to imitate Jesus Christ.
We must not scold the little boy at the seashore tossing back starfish one by one after a storm, saying, “You can’t make a difference to those thousands of starfish on the beach.” We must be like the little boy who tosses in another starfish and says, “But it made a difference to that one.”
This approach will not change our health care system overnight, but it will begin to change the lives of numerous patients by healing the physicians, one-by-one, who treat them.



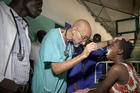
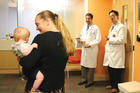






Indeed, doctors must be physically fit to make sure that they really put to practice what they thought. I think its harder for a doctor to say that we must have lean body through exercise and such when the doctor himself is too big and fat.
Scott Porter(West Palm Beach digital agency)