The case of Charlie Gard case is disturbing because it represents a blurred line between euthanasia and palliative care—and I think that no one in this case wants to be accused of euthanasia. The parents, health care professionals and court officials all clearly want to do what is right. As with so many things, though, “what is right” depends very much on how we tell the story.
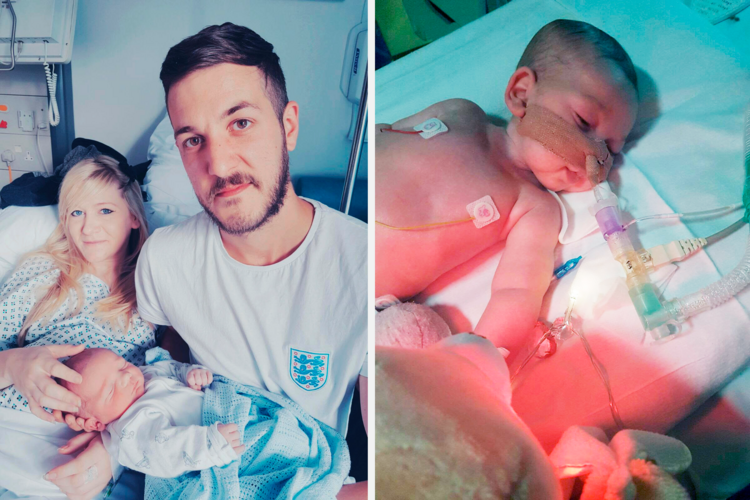
For many, Charlie is a dying boy whose quality of life is in question, and who is probably feeling pain from the ventilation system that enables him to breathe. As the decision by Britain’s highest court notes, the medical professionals caring for Charlie believe that “[he] can probably experience pain, but is unable to react to it in a meaningful way. Their evidence was that being ventilated, being suctioned, living as Charlie does, are all capable of causing pain.”
The Charlie Gard case is disturbing because it represents a blurred line between euthanasia and palliative care.
In this context, the Catholic Church’s distinction between ordinary means and extraordinary means of prolonging life and seeking treatment makes sense, as it appears there are no “ordinary” treatments available to Charlie given his condition. St. John Paul II wrote in “Evangelium Vitae”: “It needs to be determined whether the means of treatment available are objectively proportionate to the prospects for improvement. To forego extraordinary or disproportionate means is not the equivalent of suicide or euthanasia; it rather expresses acceptance of the human condition in the face of death” (No. 65). The courts have determined that the available treatment is not objectively proportionate and that Charlie, suffering from a rare genetic condition called infantile onset encephalomyopathic mitochondrial DNA depletion syndrome, or M.D.D.S., should instead receive palliative care.
Yet there is another story here. That story is the court’s repeated and consistent allusion to Charlie’s mental disability and brain damage as a key reason for not attempting the experimental treatment that the parents have sought—treatment that a doctor in the United States is willing to attempt and that people have supported with their funding. (On Friday, the Great Ormond Street Hospital said it would reconsider its decision to turn off life support for Charlie Gard and would seek a new ruling from the courts in light of “new evidence” about possible treatment.)
The focus of the court’s documents is not on Charlie’s imminent death, but on his brain function.
The decision by the Royal Courts of Justice, upheld by the European Court of Human Rights, even notes that Great Ormond Street Hospital staff had entertained the experimental procedure: “At one stage, Great Ormond Street Hospital got as far as deciding to apply for ethical permission to attempt nucleoside therapy here—a treatment that has never been used on patients with this form of MDDS—but, by the time that decision had been made, Charlie’s condition had greatly worsened and the view of all here was that his epileptic encephalopathy was such that his brain damage was severe and irreversible that treatment was potentially painful but incapable of achieving anything positive for him.” It is not entirely clear what “positive” might mean here, but the decision links “positive” with mental state. The court decision later notes: “But if Charlie’s damaged brain function cannot be improved, as all seem to agree, then how can he be any better off than he is now, which is in a condition that his parents believe should not be sustained?”
The focus of the court’s documents is not on Charlie’s imminent death, but on his brain function. That does not, to me, mandate what “Evangelium Vitae” calls the “acceptance of the human condition in the face of death.” Rather, it suggests to me our own societal failure to accept people with disabilities, including and especially mental disabilities.
The church has something to say about that, too. In “Evangelium Vitae,” the pope writes about prenatal diagnostic techniques that encourage selective abortion with respect to babies who might have disabilities, including disabilities like the ones Charlie has: “Such an attitude is shameful and utterly reprehensible, since it presumes to measure the value of a human life only within the parameters of ‘normality’ and physical well-being, thus opening the way to legitimizing infanticide and euthanasia as well” (No. 63). Rather, Christians are asked to live lives of solidarity with all, including those who are disabled (Catechism, 2208).
What our tests can measure about brain function is not a solid indication either of death or future quality of life. Bioethicist Jeff Bishop has shown that we have arbitrarily created guidelines about brain function that support our culture’s particular view of mental health and illness. There are numerous examples of families and medical practitioners being surprised by improvement and recovery in apparent brain death or vegetative state cases, and there is extensive research about autism and other conditions involve different kinds of brain functioning. This is all to point out that our understanding of brain health and mental well-being is limited and involves more questions than answers.
That is why, when the court’s ruling is so focused on brain function rather than imminent death, I think that the court ought to permit experimental treatment. I think Christians ought to push against the subtle (and apparently well-meaning) bias perpetuated about disabilities. And I think church teaching enables Christians to support Charlie and his parents in their desire to seek further treatment.








As a palliative care physician in London for the past 22 years, please allow me to disagree. I think the first part of the article gets it right: we are in a situation of very extraordinary means to keep someone immensely vulnerable alive which are almost certain to be causing intense suffering to which this deeply disabled baby cannot react. There was no evidence that the treatment would benefit Charlie, but it had the capacity to do harm (especially suffering) as well as good - it is an unknown. Stopping the treatment is moral in that situation; there are times when not stopping it would be immoral.
Having read many rulings of the UK superior courts where they grapple with such matters of life and death, and disability, I can assure you their approach is far more nuanced and sensitive than this article presents. They have stood in many ways in the defence of the rights of people who do not have the capacity to choose for themselves to be treated with great dignity, respect and thoughtfulness. By no means can this body of opinion over many years be reduced to "this person is deeply disabled, therefore matters less". Quite the contrary.
Having frequently been in situations where one has to decide whether or not to intervene in a situation that is not at all clear cut , and where very considerable harm may ensue from getting it wrong, the paediatricians have my every sympathy. They are not insensitive to the parents' suffering, whom they face every day. Of course, not in a way as intense as the parents, but intense and suffered deeply nonetheless, they are struggling with a very deep dilemma which is too easy for someone who has not sat in the hot seat to reduce to black and white.
The fact that the hospital applied to the Court for a revision of the judgement n the day it received unpublished evidence that these treatments might have a useful effect in conditions which have some similarities shows not only that disability is not the issue; but also that the doctors have kept agonising over the rights and wrongs of this case, because any human being who has chosen to spend one's life dealing with very disabled children and their parents facing the most complex problems, invariably would. We owe it to them, and to the parents,not to reduce them to slogans.
So you are convinced of the likelihood of evil motivations on the part of those who advocated for the life of the child and of the impossibility of bad motivations on the part of those who denied continued medical treatment, as though their mortal souls can not possibly be motivated by any level of human pride that gets to decide when a life becomes, in their judgment, no longer a life worthy of life? The sins of pride can not exist among the well educated. Ever hear of the Wansee conference?
If Charlie were breathing on his own, I might agree with the author of this article. But he isn't.
In my family, in the eighties, the same situation occurred. The parents were devastated that their baby's brain activity showed almost nothing. She would have died had she not been put immediately on a respirator. The prognosis, after a few days, was terrible: she probably would never even swallow, given the parts of the brain she was missing. The doctor said he had never seen a case like this and wanted to keep the baby on the respirator "to see how much brain growth there will be." The mother asked, "But if she's suffering in this condition of being kept alive for that medical knowledge, at what point would her suffering outweigh the value of experiment to medicine?" The doctor said "Never." The mother told me that this conversation took place in the doctor's office, which was full of miniature models of classic sports cars that he collected. Why is this pertinent? Because the doctor shamed her, saying "You're just disappointed that you didn't have a perfect Gerber baby." She felt the doctor was thinking only of himself, not of the baby being kept alive though she had almost no brain waves. She and her husband summoned our cousin, a nun, who flew to the hospital and compassionately backed up the parents' plea to the board of ethics that they be allowed to unhook their daughter from the needles and hold her in their arms for as long as she had, to say goodbye. Her father became an architect of fountains and told me that every one he ever created "has been my daughter's baptismal fount." She has never been forgotten. Grief, and admission of grief is at the center of the beautiful family they created, which includes a healthy child and a child also born with brain atrophy that was less extensive. They loved him as long as they could in his home, then moved to a state where he could get the best situation for school; he is now emancipated in an adult group home and lights up for their visits. This is true Respect for Life. I am aware of worrying about slippery slopes. But the Spirit prompts us by love, and sometimes the medical profession is impervious to those promptings. (So, too, the church.) It took consulting a lot of people for this couple to arrive at their decision. Doctrinaire opinion was not on the side of that child, body or soul. Luckily our cousin, the religious sister, bravely stood by the parents. That child's soul lives on and is connected to her loved ones. Her body could not live without all that intervention, and it was not reverent to make her a medical experiment.
Since writing my previous response I have gone back to Judge Francis' original judgment, which the article quotes brief excerpts from, and cannot hep but conclude that the author misunderstood the point the judge was making.
The judge was not saying that for a treatment to be worthwhile it had to improve the mental function of a severely mentally disabled child. Reading the full judgment, rather than the initial summary, one learns that Charlie has no spontaneous breathing activity, and would no longer breathe if the ventilator was switched off; that he has no muscle activity; that he has frequent epileptic seizures ; that repeated investigation reveals no sign of interaction or responsiveness etc. Making a child breathe who otherwise would not who then goes on to suffer probable significant pain he cannot do anything to avoid and frequent seizures... Those are the criteria in which one has to define a benefit for it to be meaningful, and that is implied by the judge's statement of the facts.
He also made clear his duties at law by quoting from a previous landmark judgment:
"In our judgment, the intellectual milestones for the judge in a case such as the present are, therefore, simple, although the ultimate decision will frequently be extremely difficult. The judge must decide what is in the child's best interests. In making that decision, the welfare of the child is paramount, and the judge must look at the question from the assumed point of view of the patient. There is a strong presumption in favour of a course of action which will prolong life, but that presumption is not irrebuttable. The term 'best interests' encompasses medical, emotional, and all other welfare issues."
He spoke to experts from various hospitals in the UK and Barcelona, and to the doctor in the USA who had offered to treat ("However, the US doctor made it clear that, were Charlie in the United States, he would treat him if the parents so desired and could pay for it. " - now there is the real ethical scandal, in that last phrase); he admitted on receiving details of the case he had no experience of treating someone with nucleosides who had encephalopathy, that this had not even been done in mice, and that there was no theoretical basis for judging whether in this situation there would be any benefit.
I fear there is currently a movement in the Catholic Church which looks at God as if he stands there, clipboard in hand, ready to condemn us should we, by making a decision in a staggeringly difficult situation, rob someone of what the US doctor proposing treatment admitted was an infinitesimal chance of improvement. I find the criteria quoted above from the previous judgement by the judge much more in line with traditional Catholic teaching on medical ethics; I fear we are lapsing, through incomprehension of the real physical suffering people face in these totally dreadful situations, into a kind of fundamentalism about sustaining life at all costs that will only alienate many people of good will, for all the right reasons. I speak as very much a Catholic.
thank you for this. I do not see disability bias in the decisions of the doctors but do see a bias in the argument of the author. It is not about what constitutes meaningful life ~ it is about recognizing that the baby's machine controlled bodily responses are not equivalent to living. Saying "enough" is a tremendously difficult decision and one that seems beyond the ability of these parents. Someone needs to say it for them and support them as they let go.
Thanks to Doctor Pace for his sensitive and helpful comments.
Thank you Dr. Pace for your thoughtful and illuminative comments. I agree with you that the case of Charlie Gard has nothing to do with disability bias. The author's analysis is incorrect. Taking poor Charlie off of a respirator and letting nature take its course is forgoing extraordinary means. To suggest that this could be euthanasia is misguided. It is heartbreaking for Charlie's parents to face this situation. Who among us could easily let go of our 11 month old child and yet I know from my Catholic faith that love sometimes means letting go. I am not sure that subjecting Charlie to the experimental treatment that Columbia Presbyterian has offered to make available to Charlie at the Great Ormond Street Hospital makes sense. The unknown effects of this treatment may add to the pain he probably already is experiencing. At the end of the day, Charlie Gard will still be dying. We need to surround Charlie's parents with our thoughts and prayers. They will need strength to let their sweet boy go and rest in the arms of God where there will be no more pain.
What is this child's quality of life if the treatment is successful? It's clear that the quality is very poor with a remote possibility of success, it's not a question of disability discrimination.
Thanks to Dr. Pace for his thoughtful and enlightening comments. Having cared for an infant with a mitochondrial disorder, I was shocked by how little of life remained for the child. She was breathing on her own, but continual seizures robbed her of consciousness in the usual sense. Purposeful movement was absent. Her condition was expected to deteriorate till her death while still an infant.
An experimental treatment that has not even been tried on mice could kill a child by itself, to say nothing of failing to do any good. The likelihood of restoring brain function to the point that Charlie Gard could breathe on his own is small. Allowing the parents to take him home and care for him until his death would be the kindest option.
Until a person sees this kind of condition with their own eyes, it is hard to fathom. To assume that those treating Charlie Gard are biased in their decision-making is unfair. It is a heartbreaking situation for all involved, including the doctors and other caregivers. Onlookers have little right to comment negatively until they have walked in the shoes of those trying their best to make sound, ethical decisions while providing care.
For me the question at the heart of this issue would seem to be: WHY IS A COURT MAKING THIS MOST FINAL OF DECISIONS INSTEAD OF THE PARENTS?
It is fairly astounding that as a result of the UN Treaty on Human Rights signed by Great Britain that this child'destiny WAS/is in every respect being controlled by a Court, including his parents rights to take him out of Great Ormond Hospital.